When is a problem not a problem?
Refusing to dispense drugs to kill patients with psychiatric illness
Levenseinde Kliniek complains about uncooperative Dutch pharmacists
Sean Murphy*
Full Text

In April, 2014, a complaint was made in the
Netherlands that some Dutch pharmacists were refusing to provide euthanasia
drugs. The complaint led members of the Dutch Parliament from the
green party, GroenLinks, to ask for a debate with health minister, and
members of other Dutch political parties let it be known that they were also
concerned.1
According to the news reports,
over half the physicians at "the independent euthanasia clinic" had been
refused lethal drugs, and 23 percent of 53 pharmacists surveyed reported
that they sometimes refused to fill euthanasia prescriptions. It was argued
that pharmacists should not be able to refuse drugs needed to kill patients
if two physicians had approved the euthanasia request.2
However, while the law in the Netherlands permits physicians to provide
euthanasia, it does not mention pharmacists.
Note that excitement among GroenLinks party
members and other politicians and the subject of the news reports was the
experience of physicians at a single "independent euthanasia clinic," which
the English language report did not identify. It was, in fact, the
Levenseinde Kliniek (End of Life Clinic)(LK) in Amsterdam.1,2
The facility has an interesting history. It begins with what seems to
be the reluctance of many Dutch physicians to personally kill patients.
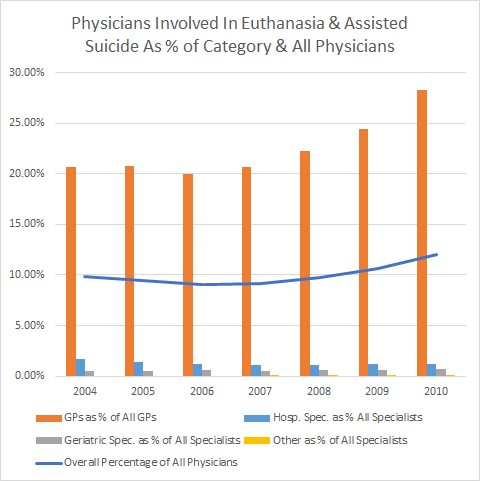
Statistics indicate that a maximum of 9% to 12% of
all Dutch physicians have been directly involved in reported euthanasia
cases each year (Appendix "A"),
though the proportion of general practitioners who personally kill patients
is much higher: 28% in 2010. It must be emphasized that, while these
figures are approximate, they are approximate maximums.
Official statistics are not compiled in a way that makes it possible to
determine whether ten patients have been killed by ten physicians, or by
only one.
Taking a different perspective, the statistics
suggest that at least 88 to 91% of Dutch physicians (or at least 72% of
general practitioners) do not kill patients themselves. This
likely explains the complaint by Dr. Petra de Jong of Right to Die-Nl that
"many general practitioners, either for moral reasons or perhaps because of
uncertainty about the law," refuse to perform euthanasia.3
Moreover, though the Royal Dutch Medical Association claims that physicians
who refuse to kill patients themselves are obliged to refer patients to
someone who will,4 it seems (according
to Dr. de Jong) that many will not do so.5 For these
reasons, in 2012, Right to Die NL formed mobile teams to provide euthanasia
for patients at home. The
Levenseinde Kliniek (End of Life Clinic) in Amsterdam was established to
provide the teams with a base of operations.
Eric van Wijlick, a policy adviser for the Royal Dutch Medical
Association, expressed uneasiness about the mobile teams when Levenseinde
Kliniek was established. He did not care for the practice of separating the
provision of euthanasia from ongoing care by a general practitioner. If a
physician refuses euthanasia, he said, it is usually for a good reason,
such as failing to meet legal criteria for the procedure. In contrast,
those running Levenseinde Kliniek believe that everyone over 70 years old
should be allowed to have euthanasia if they are tired of living.3
Van Wijlick's misgivings seem justified in light of some of practices of
the mobile teams. In April, 2014 - as GroenLinks and others were
fretting about uncooperative pharmacists - government officials
criticized a Levenseinde Kliniek physician who lethally injected an elderly
woman with psychiatric problems because he did not talk to her enough. Four
months later, Levenseinde Kliniek was reprimanded by euthanasia monitoring
officials for killing a stroke victim in her 80's. She was said to be
"suffering unbearably" because she did not want to live in a nursing home.6
This information provides a broader context for
the evaluation of the "problem" attributed to pharmacists who refused to
fill prescriptions for LK physicians. In most cases, refusals were
based on pharmacists' religious beliefs or involved patients with
dementia, psychiatric illness, or who simply consider their lives complete
and wish to die.1 In other words,
the objecting pharmacists appear to have been acting upon the same kinds of
concerns that led Dutch authorities to reprimand the facility.
The Royal Dutch Pharmacists Association
(Koninklijke Nederlandse Maatschappij ter bevordering der Pharmacie, KNMP)
defended pharmacists who were unwilling to dispense lethal medications for
euthanasia: "A pharmacy is not a shop where deadly drugs are just handed over."1
Speaking for the Association, Annemieke Horikx
complained about the attitude of some physicians:
They say, "Get me the
medication and be quick about it". That's no way to request medication.
These are matters of life and death we're dealing with. We also hear from
pharmacists that the doctors concerned are unknown to them.1
Unfortunately, the KNMP accepted the
characterization of Levenseinde Kliniek's difficulties in getting lethal
drugs as a problem to be solved, and offered a solution. This is a
classic example of getting the wrong answer by beginning with the wrong
premise. There was a conflict, to be sure, but, as official criticism
of Levenseinde Kliniek indicates, it is by no means clear that the refusal
of some pharmacists to supply some LK physicians was problematic. It
may, in fact, have been more in keeping with the law and medical ethics than
the conduct of the LK physicians.
In any case, the KNMP proposed that Dutch law
should be amended to recognize the role of pharmacists in euthanasia, and
added that objecting pharmacists should refer physicians to a pharmacy
willing to dispense euthanasia drugs.1
Faced with the "problem" of pharmacists who refuse to dispense drugs
to kill patients with psychiatric problems or dementia, or elderly people
who dislike nursing homes, the "solution" proposed by the KNMP is to force
the objectors to find a colleague willing to do so.
From the perspective of freedom of
conscience, this cure is as bad as the disease.
The Dutch officials who reprimanded Levenseinde
Kliniek might even say it is worse.
Netherlands: Termination of Life on Request and Assisted Suicide (Review Procedures)
Act
Euthanasia and assisted suicide were legalized in the Netherlands in 2002. The following
statistics refer only to reported euthanasia and assisted suicide cases.
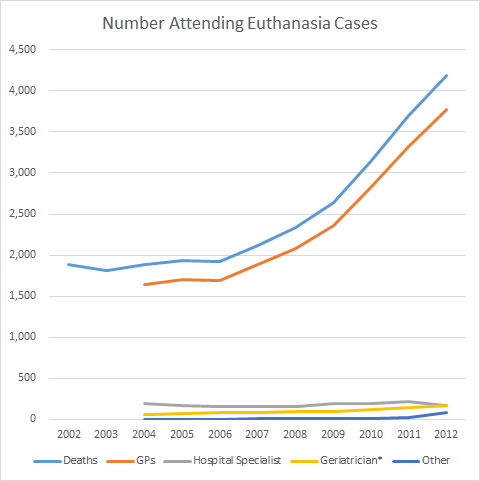
Note that there is no way to determine from the statistics provided how
many times a physician acted as a consultant in different euthanasia cases
throughout the year. A single physician involved in three cases will
appear here as three physicians. Thus, the statistics here indicate
the maximum number of physicians involved in reported cases each year, not
the actual number of physicians participating.
| |
Deaths |
Attending Physician |
| Year |
Total |
Euthanasia |
A.
Suicide |
Combined |
GP |
Hospital Specialist |
Geriatrician* |
Other |
Total |
|
2002 |
1,882 |
|
|
|
|
|
|
|
|
|
2003 |
1,815 |
1,626 |
148 |
41 |
|
|
|
|
|
|
2004 |
1,886 |
1,714 |
141 |
31 |
1,646 |
188 |
52 |
0 |
1,886 |
|
2005 |
1,933 |
1,765 |
143 |
25 |
1,697 |
170 |
66 |
0 |
1,933 |
|
2006 |
1,923 |
1,765 |
132 |
26 |
1,692 |
151 |
80 |
0 |
1,923 |
|
2007 |
2,120 |
1,923 |
167 |
30 |
1,886 |
157 |
76 |
1 |
2,120 |
|
2008 |
2,331 |
2,146 |
152 |
33 |
2,083 |
152 |
91 |
5 |
2,331 |
|
2009 |
2,636 |
2,443 |
156 |
37 |
2,356 |
184 |
87 |
10 |
2,637 |
|
2010 |
3,136 |
2,910 |
182 |
44 |
2,819 |
193 |
115 |
9 |
3,136 |
|
2011 |
3,695 |
3,446 |
196 |
53 |
3,329 |
212 |
139 |
15 |
3,695 |
|
2012 |
4,188 |
3,965 |
185 |
38 |
3,777 |
171 |
166 |
74 |
4,188 |
Sources: Regional Euthanasia Review
Committees Annual Reports.
Note: *Includes
physicians working in nursing homes.
Click to enlarge
| |
|
Total in
Netherlands/Category |
Percentage of Totals,
Categories & Overall |
| Year |
Deaths |
GP |
Med. Spec. |
Physicians |
%GP |
%HS |
% Geriatric |
%Other |
%Overall |
|
2004 |
1,886 |
7,960 |
11,275 |
19,235 |
20.68% |
1.67% |
0.46% |
0.00% |
9.81% |
|
2005 |
1,933 |
8,165 |
12,305 |
20,470 |
20.78% |
1.38% |
0.54% |
0.00% |
9.44% |
|
2006 |
1,923 |
8,450 |
12,850 |
21,300 |
20.02% |
1.18% |
0.62% |
0.00% |
9.03% |
|
2007 |
2,120 |
9,130 |
14,080 |
23,210 |
20.66% |
1.12% |
0.54% |
0.01% |
9.13% |
|
2008 |
2,331 |
9,350 |
14,485 |
23,835 |
22.28% |
1.05% |
0.63% |
0.03% |
9.78% |
|
2009 |
2,636 |
9,660 |
15,020 |
24,680 |
24.39% |
1.23% |
0.58% |
0.07% |
10.68% |
|
2010 |
3,136 |
9,960 |
16,055 |
26,015 |
28.30% |
1.20% |
0.72% |
0.06% |
12.05% |
Sources: Regional Euthanasia Review
Committees Annual Reports; Statistics Netherlands:
Health, lifestyle, health care use and supply, causes of death; from 1900.
Subjects:
Care Supply, Health Professions. (Accessed 2014-07-16)
Note: percentages of hospital and
geriatric specialists and "other" is relative to the total number of medical
specialists. Overall percentage is in relation to total number of
physicians.
Click to enlarge
Notes
1. DutchNews.nl, 16 April, 2014
"Pharmacists sometimes refuse to give doctors euthanasia drugs." (Accessed 2014-10-24)
2. nrc.nl nieuws, 16 April, 2014.
"Apothekers weigeren soms middelen voor euthanasie te leveren." (Accessed 2014-10-24)
3. Jolly D.,
"Push for the Right to Die Grows in the Netherlands." New York
Times, 2 April, 2012. (Accessed 2014-07-15)
4. Royal Dutch Medical Association,
The Role of the Physician in the Voluntary Termination of Life
(30 August, 2011), p. 40 (Accessed 2012-07-12)
5. Brumfield, B. "Dutch euthanasia clinic offers mobile service." CNN,
9 March, 2012 (Accessed 2014-07-15)
6. DutchNews.nl "Euthanasia
clinic reprimanded for death of stroke victim." 27 August, 2014.
(Accessed 2014-11-05)